|
ECG and telemetry were double-checked by a cardiac surgeon and an electrophysiologist. Even without telemetry, episodes of AF were detected by a change in clinical status, which led to an immediate bedside electrocardiogram. After the telemetry was removed, a standard 12-lead ECG was routinely recorded on the first and third day after leaving the ICU. All patients underwent continuous ECG monitoring in the ICU for at least 48 h postoperatively. This standard is consistent with most previous studies. POAF was defined as any episode of atrial fibrillation (AF) (occurrence of irregular heart rhythm, without detectable P waves) lasting more than 30 s on cardiac telemetry or requiring treatment (including antiarrhythmic drugs, such as amiodarone or electrical cardioversion) during hospitalization. The primary outcome was the occurrence of new-onset POAF, as a binary value. This study was conducted following the Declaration of Helsinki and its amendments. All identifiable information about the patients was hidden, and their identities could not be determined based on context. Given the observational nature of this study, the requirement for informed consent was waived. The study was approved by the institutional review board of the Chinese PLA General Hospital (approval number S2022-360-01). The final sample consisted of 1587 patients. The exclusion criteria were: age < 18 years, incomplete or non-availability of medical records, non-sinus electrocardiogram before surgery, medical history of atrial fibrillation or atrial flutter, pacemaker implantation, history of radiofrequency ablation or Cox maze procedure for arrhythmia, and death during the perioperative period. Elective, urgent, and emergency procedures were also performed. The surgery types included isolated coronary artery bypass grafting (CABG), valve surgery, concomitant valve and CABG, and valve and ascending aorta surgery. This retrospective study included 2108 consecutive adult patients (age ≥ 18 years) who underwent cardiac surgery at the First Medical Center of Chinese PLA General Hospital (Beijing, China) from January 2018 to December 2020. To our knowledge, this is the first study to compare different algorithms for developing a POAF risk model. 
Machine learning and logistic regression algorithms were used to develop a predictive model. Our study aimed to develop a simple yet valid risk assessment model to predict POAF after cardiac surgery. Several predictive models have been developed to achieve this goal. Identifying patients prone to POAF makes personalized prophylactic treatment feasible. In contrast, POAF prophylaxis can cause hypotension, bradycardia, or heart block. Additionally, POAF increases hospitalization length and costs. It has been found that POAF after cardiac surgery is associated with a substantial risk of adverse outcomes, including increased mortality, postoperative stroke, respiratory infections, and gastrointestinal dysfunction. New-onset atrial fibrillation, including paroxysmal, persistent, or permanent after any heart surgery, may be classified as POAF. New-onset postoperative atrial fibrillation (POAF) is the most common complication after adult cardiac surgery, with a reported incidence rate from 15 to 50%. We developed a nomogram that may assist clinicians in identifying individuals who are prone to POAF. Logistic regression performed better than machine learning in predicting POAF. The calibration curve of the new model was relatively well-fit ( p = 0.502). A simple bedside tool comprising three variables (age, left atrial diameter, and surgery type) was established, which had a discriminative ability with a ROC of 0.726 (95% CI 0.693–0.759) and 0.727 (95% CI 0.676–0.778) in derivation and validation subsets respectively. Logistic regression provided the highest area under the receiver operating characteristic curve (ROC) in the validation cohort. POAF was observed in 414 hospitalized patients. 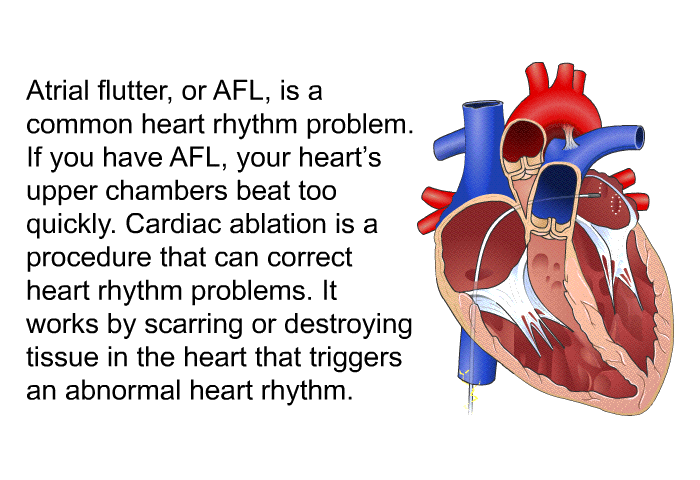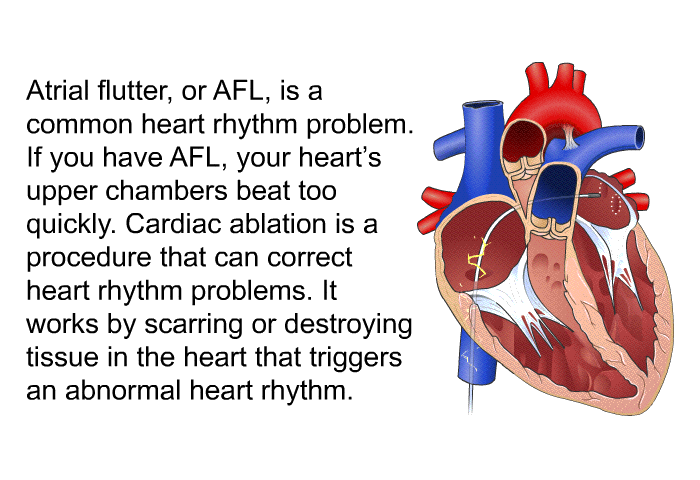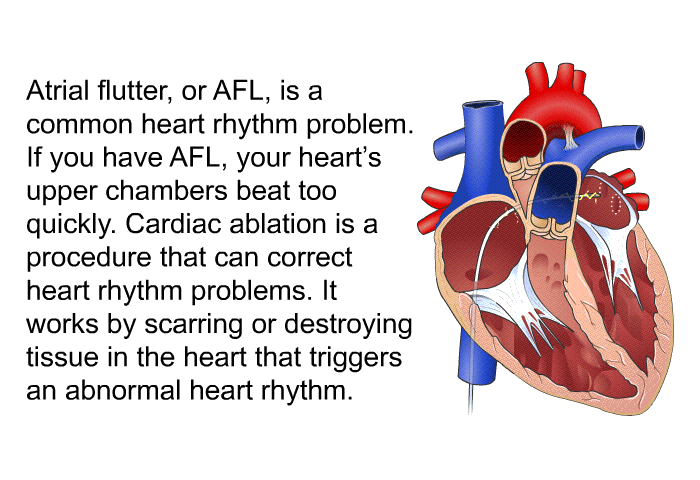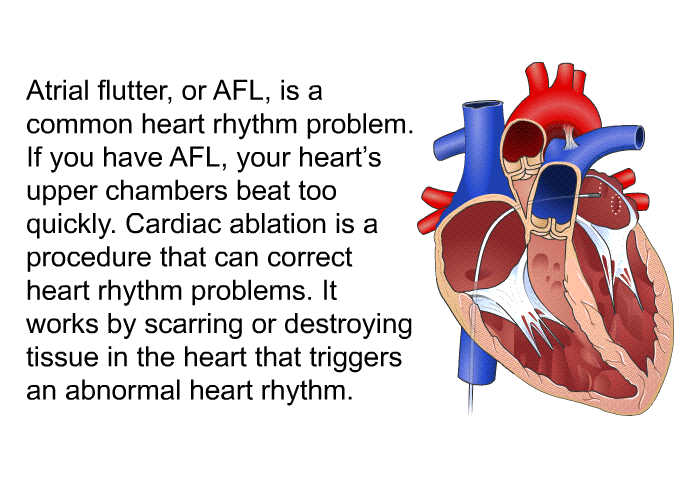
We also developed a simple nomogram based on the strength of the results and compared its predictive ability with that of the CHA2DS2-VASc and POAF scores currently used in clinical practice. Logistic regression or machine learning methods were applied to predict POAF incidence from a subset of 123 parameters. The types of surgery included isolated coronary artery bypass grafting, valve surgery, combined valve and coronary artery bypass grafting (CABG), or aortic surgery. We retrospectively analyzed the data of 2108 consecutive adult patients (> 18 years old) who underwent cardiac surgery at our medical institution. This study aimed to develop a new nomogram to predict POAF using preoperative and intraoperative risk factors. New onset postoperative atrial fibrillation (POAF) is the most common complication of cardiac surgery, with an incidence ranging from 15 to 50%.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
